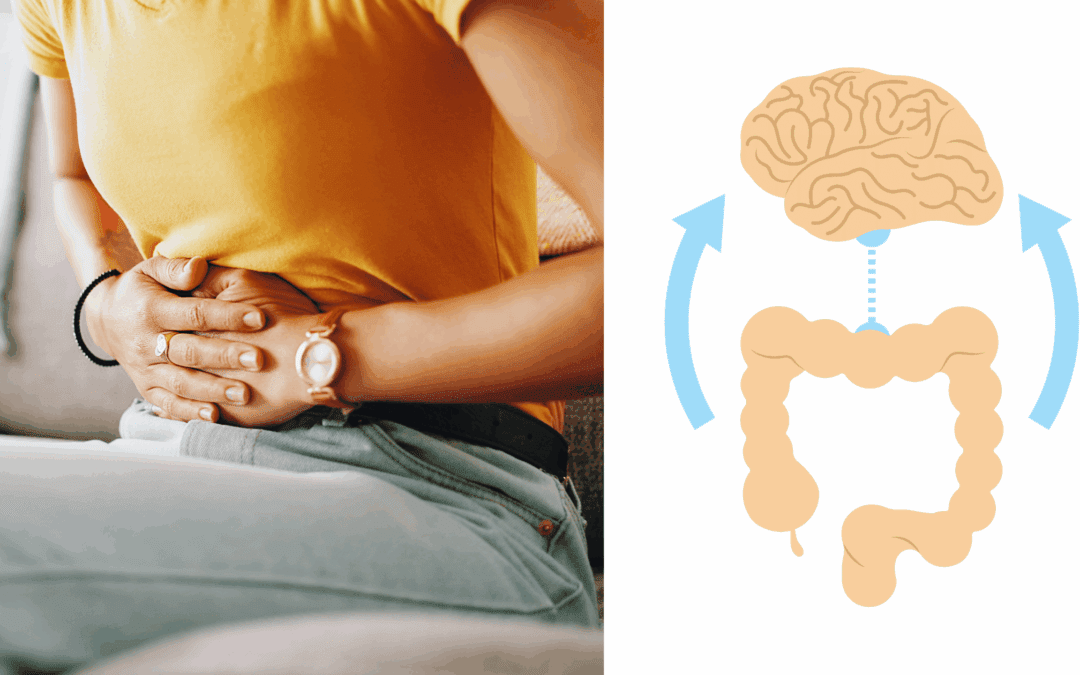
IBS and the Gut–Brain Axis: Why Stress Affects Your Digestion
If you live with Irritable Bowel Syndrome (IBS), you may already notice a pattern:
- Your gut behaves differently during stressful periods.
- Symptoms flare before important events
- Digestive discomfort appears even when you’re eating well
For many people, this leads to a frustrating question:
“Is my IBS caused by stress?”
The answer is nuanced.
IBS is increasingly understood as a condition involving the gut–brain axis, a complex communication system linking your digestive system, nervous system, immune system and gut microbiome.
Understanding this connection helps explain why IBS symptoms happen and why effective care often needs to support both gut health and nervous system regulation
Author: Norelle Hentschel (Master of Advanced Naturopathic Medicine).
This information is general in nature and does not replace individual medical advice. If you are experiencing severe, persistent or unusual symptoms, please seek medical care.
Quick Summary: The Gut-Brain Axis and IBS
- IBS is now understood as a disorder of gut–brain interaction, not just a digestive condition.
- Your gut and brain communicate constantly through nerves, hormones, immune signals and gut microbes.
- Stress can influence digestion by changing gut motility, sensitivity and inflammation.
- The gut microbiome helps regulate neurotransmitters such as serotonin, which affect both mood and bowel function.
- Many IBS symptoms occur because the gut becomes more sensitive, not because damage is present.
- Effective IBS support often involves addressing both digestive health and nervous system regulation.
What Is the Gut–Brain Axis?
The gut and brain are constantly communicating.
Scientists refer to this connection as the gut–brain axis which is a two-way communication network between:
- The brain and central nervous system
- The digestive tract
- The immune system
- The trillions of microbes living in the gut
Rather than the brain simply controlling digestion, information flows in both directions.
Your thoughts, emotions and stress responses influence digestion.
At the same time, signals from the gut influence mood, pain perception and overall wellbeing.
This is why the gut is often called the body’s “second brain.”
Credit: Suganya, Kanmani, and Byung-Soo KooThinkpinsMister PommeroyVectorization: Mrmw, CC BY-SA 4.0
How the Gut and Brain Talk to Each Other
Communication within the gut–brain axis occurs through three main pathways.
1. The Nervous System
Your digestive tract contains its own specialised nervous system called the enteric nervous system.
This network communicates directly with the brain through nerves such as the Vagus nerve and helps regulate:
- bowel motility
- digestive secretions
- sensation within the gut
In IBS, this signalling system can become more sensitive, meaning normal digestive activity may feel uncomfortable or painful.
2. Hormonal and Stress Pathways
When the brain perceives stress, it activates the body’s stress response system (often called the HPA (hypothalamic pituitary adrenal) axis.
Stress hormones such as cortisol influence digestion by:
- altering gut motility
- changing intestinal permeability
- affecting immune activity
- modifying communication between gut nerves and the brain
This doesn’t mean IBS is psychological. It means stress has real, measurable effects on digestive physiology.
3. The Immune System
The gut contains a large proportion of the body’s immune cells.
Low-grade immune activation and inflammatory signalling are increasingly recognised features of IBS. These immune signals interact closely with gut nerves, influencing sensitivity, motility and symptom severity.
The Role of the Gut Microbiome in IBS
Your gut microbiome, the community of bacteria, fungi and other microorganisms living in the digestive tract plays a central role in the gut–brain axis.
Research suggests many people with IBS have differences in:
- microbial diversity
- bacterial balance
- microbial metabolic activity
Importantly, there is no single “IBS microbiome.”
Instead, individual patterns vary widely, which helps explain why IBS looks different from person to person.
Gut microbes help produce compounds that influence:
- intestinal barrier health
- immune regulation
- inflammation levels
- communication with the nervous system
They even participate in producing chemical messengers traditionally associated with the brain.
Your Gut Produces Brain Chemicals
One of the most surprising discoveries in modern medicine is how closely digestion and neurotransmitters are linked.
Serotonin
Around 90-95% of serotonin is produced in the gut.
Serotonin helps regulate:
- bowel movement speed
- intestinal sensation
- secretion within the digestive tract
Altered serotonin signalling is strongly linked with both diarrhoea-predominant and constipation-predominant IBS.
GABA and Other Neurotransmitters
Certain gut microbes help influence the production of calming neurotransmitters such as GABA, as well as dopamine and noradrenaline.
These chemicals affect:
- pain perception
- gut motility
- stress responsiveness
This helps explain why digestive symptoms and mood often influence each other.
Why IBS Can Feel So Painful: Visceral Hypersensitivity
Many people with IBS experience something called visceral hypersensitivity.
This means the gut’s nerves become more reactive.
Normal digestive processes such as gas movement, bowel contractions or stretching of the intestine may be interpreted by the nervous system as pain or urgency.
Importantly, this does not mean damage is present.
Rather, the gut–brain communication system has become overly alert.
The Role of Stress in IBS Flares
Almost all gastrointestinal conditions are influenced by stress, but IBS appears particularly sensitive to it.
Stress can:
- change gut motility
- increase intestinal sensitivity
- influence the microbiome
- activate immune cells called mast cells
- alter neurotransmitter release
Over time, this can create a feedback loop:
Gut symptoms increase stress → stress worsens gut signalling → symptoms intensify.
Breaking this loop is often a key part of improving IBS symptoms.
Why IBS Is Different for Everyone
IBS is now considered a disorder of gut–brain interaction, meaning multiple systems contribute to symptoms.
Factors that may influence IBS include:
- microbiome composition
- past gastrointestinal infections (post-infectious IBS)
- stress exposure
- hormonal influences
- nervous system regulation
- genetics and early life factors
Because of this complexity, there is rarely a single trigger or universal solution.
What This Means for Treatment
Understanding the gut–brain axis has changed how IBS is managed.
Rather than focusing only on suppressing symptoms, modern approaches aim to support communication between the gut, nervous system and immune system.
A comprehensive IBS management plan may involve:
Supporting Digestive Function
- individualised dietary strategies
- appropriate fibre intake
- supporting microbial balance
- reducing gut irritation
Supporting the Nervous System
- stress regulation strategies
- sleep optimisation
- gentle nervous system support
- mind–gut therapies
Supporting Gut–Immune Balance
- addressing low-grade inflammation
- improving gut barrier function
- personalised nutritional and lifestyle support
Care is always individualised based on symptoms, history and overall health.
The take home message
IBS is not “just stress.”
And it is not simply a bowel problem either.
IBS reflects a complex interaction between:
- the gut
- the brain
- the immune system
- and the microbiome
When this communication becomes disrupted, symptoms such as pain, bloating, diarrhoea or constipation can develop even when medical tests appear normal.
The encouraging news is that by supporting the gut–brain axis, many people experience meaningful improvements in digestive comfort, resilience to stress and overall wellbeing.
Because IBS is rarely caused by a single factor, care that considers both digestive and nervous system health can be an important step toward long-term symptom stability.
How Naturopathy Can Support the Gut–Brain Connection
Because IBS involves communication between the gut, nervous system and immune system, naturopathic care focuses on supporting multiple body systems together.
Treatment is always individualised, but support may include:
🌿 Supporting Immune and Gut Barrier Health
The intestinal lining plays an important role in immune regulation and nervous system signalling. Nutritional and herbal strategies may be used to help support:
- healthy intestinal barrier function
- balanced immune responses
- reduction of low-grade gut inflammation
🌿 Stress-Modulating Herbal Support
Since stress signalling strongly influences IBS symptoms, selected herbs traditionally used in Western herbal medicine may help support:
- nervous system resilience
- healthy stress responses
- sleep quality and relaxation
These herbs aim to support regulation rather than simply suppress symptoms.
🌿 Carminative Herbs for Digestive Comfort
Carminative herbs have traditionally been used to ease digestive discomfort and support motility.
They may assist with:
- gas and bloating
- abdominal cramping
- digestive stagnation
By improving digestive comfort, these herbs may indirectly help calm gut–brain signalling pathways.
🌿 Selective Fibre, Prebiotics and Probiotics
IBS management increasingly recognises that the type of fibre matters more than the amount.
Individualised strategies may include:
- gentle or selective fibres
- prebiotics that nourish beneficial microbes
- targeted probiotic strains where appropriate
These approaches aim to support microbial balance and metabolite production involved in gut–brain communication.
🌿 Lifestyle Strategies That Support the Gut–Brain Axis
Daily habits play a powerful role in regulating gut signalling.
Support may include:
- stress regulation practices
- meal timing and eating behaviours
- sleep optimisation
- movement and nervous system regulation strategies
Small, consistent changes often have meaningful effects over time.
Ready to Take the Next Step on your IBS journey?
If you’re living with ongoing digestive symptoms, working with a practitioner who understands the gut–brain connection can help you better understand your triggers and develop a personalised plan.
At Your Remedy Naturopathy, IBS care focuses on evidence-informed, individualised support addressing both digestive and nervous system health.
Book a one-on-one appointment focused on you — your symptoms, your history and your goals. You can also select a FREE Discovery Call if you’ve got more questions
📚 Top IBS Resources
If you’d like to learn more about holistic naturopathic approaches to IBS these articles may help.
These articles reflect the clinical framework I use in practice.
How to increase fibre without bloating
Bloating when increasing fibre is a common barrier for many people. Based on my clinical practice this detailed guide provides practical strategies to help you boost fibre.
👉🏻 Read – How to increase fibre without bloating – A naturopath’s guide
5 Best Herbal Teas for Bloating
Bloating is a symptom frequently reported by people with IBS and herbal teas are an inexpensive and effective way to provide relief.
👉🏻 Read: The 5 best hebal teas for bloating
Health benefits of resistant starch - Your ultimate guide
An in-depth guide to the benefits of resistant starch for your micorbiome plus practical tips and what foods to includes in your diet.
👉🏻 Read: Health benefits of Resistant Starch
Frequently asked IBS and Gut Brain Axis Questions
Is IBS caused by stress or anxiety?
IBS is not simply caused by stress or anxiety. However, stress can strongly influence symptoms because the gut and brain communicate constantly through the gut–brain axis. Stress hormones can change gut motility, sensitivity and immune activity, which may trigger symptom flares in people already prone to IBS. This means IBS symptoms are real physiological responses — not “just psychological.”
Why do my IBS symptoms worsen during stressful periods?
When the body experiences stress, the nervous system activates changes designed for survival rather than digestion. Blood flow, hormone release and nerve signalling shift, which can alter bowel movements, increase bloating or heighten pain sensitivity. For people with IBS, the gut–brain axis may be more reactive, making the digestive system particularly sensitive to emotional or physical stressors.
Can gut bacteria affect mood or digestion?
Yes. Gut microbes produce and influence chemical messengers involved in both digestion and nervous system signalling. These include compounds that affect serotonin, inflammation and immune regulation. Changes in the gut microbiome may therefore influence digestive symptoms as well as mood, energy and stress resilience.
Why do IBS symptoms occur even when medical tests are normal?
IBS is considered a disorder of gut–brain interaction rather than a structural disease. Standard investigations often look for inflammation, infection or tissue damage. In IBS, symptoms are usually related to altered communication between gut nerves, the brain, immune system and microbiome — changes that are functional rather than visible on routine testing.
Can supporting the gut-brain axis improve IBS symptoms?
Many modern IBS management approaches focus on supporting communication between the digestive system and nervous system. This may include dietary strategies, stress regulation, microbiome support and lifestyle interventions tailored to the individual. Because IBS varies between people, personalised care is important.
How much does a consultation cost?
Consultation fees are transparent and available before booking. Fees are for consults only. Any products purchased from the dispensary are an additional cost.
The current consultation fees can be found on the Book a consult page. Naturopathy is not covered by Medicare. Some private health insurance funds offer rebates for Naturopathy. Check with your fund for details.
If you want more information before booking I also offer a free Discovery Call.

If you’re looking for a holistic, integrative approach to manage your IBS Your Remedy Naturopathy can help.
Norelle Hentschel is an experienced Naturopath with a clinic in Stones Corner, Brisbane and Telehealth consults Australia-wide. She has supported hundreds of people improve their digestive health using an evidenced based diet, lifestyle and herbal medicine approach.
Clinical review and authorship
This page has been written and reviewed by Norelle Hentschel (Master of Advanced Naturopathic Medicine) a degree-qualified naturopath based in Brisbane.
Content is informed by traditional naturopathic principles, current nutrition and IBS research, and over a decade of clinical experience.
Information provided is for educational purposes and does not replace medical diagnosis or treatment. Individual care plans are tailored in collaboration with your healthcare team where appropriate.
Last reviewed on 13 May 2026